Estonian health care system
In Estonia, there is a unified national health insurance. This means that the funds for common health insurance come from a 13% health insurance contribution deducted from the salaries of employed individuals. The health insurance contributions and access to necessary assistance are not dependent on age, income, or health risks. All insured individuals in Estonia have the right to receive equal and high-quality healthcare services.
The Estonian Health Insurance Fund covers the medical expenses of insured individuals. To achieve this, the Health Insurance Fund enters into agreements with healthcare service providers (such as general practitioners, hospitals, etc.). Providers who have signed such agreements become partners of the Health Insurance Fund. When an insured individual seeks medical consultation or treatment from a partner of the Health Insurance Fund, the Fund reimburses the cost of healthcare services.
With the agreement, healthcare facilities commit to maintaining agreed-upon waiting times, providing healthcare services according to international quality standards, and other obligations.
The list of healthcare services eligible for reimbursement by the Health Insurance Fund is approved by the government decree and is updated annually. Health insurance covers the majority of medical-related expenses. However, in certain cases, patients are required to contribute to the cost, known as patient co-payment. This includes fees for visits and hospital stays. Additionally, not all possible healthcare services are covered by the health insurance budget; only those listed in the healthcare services catalog and medically indicated for the individual.
It is important to note that the Health Insurance Fund only reimburses for healthcare services covered by a signed agreement with the healthcare facility. Upon entering into the agreement, the healthcare facility gains the right to treat individuals insured with the Health Insurance Fund's insurance money, and this information must be visibly displayed for all patients. Simultaneously, the agreement imposes obligations on the healthcare facility to adhere to agreed-upon waiting times, provide healthcare services according to international quality standards, and more.
The Estonian Health Insurance Fund receives funds from the social tax's health insurance portion (13%). From this, the Fund pays for healthcare services and health examinations provided to the insured based on agreements with healthcare institutions. All various services received for the health insurance contribution are included in the so-called treatment package, which the Health Insurance Fund reimburses. Sometimes, people mistakenly assume that health insurance covers all medical-related expenses. While the majority of healthcare services are fully covered by the Health Insurance Fund, for some services and medications, patients need to contribute partially.
Services partially or fully reimbursed for the insured include:
Partial or full payment for healthcare services to healthcare institutions, including doctor or nurse consultations, examinations, treatment procedures, preventive activities, surgeries, etc.
Providing access to more affordable medications for the insured, i.e., benefits for pharmacies for discounted medications (see also the page on discounted medications).
Reimbursement for medical devices, such as glucose meter test strips, medical devices installed during or after surgery, etc. The precise list is available on the medical devices page.
Financial benefits for the insured, such as temporary incapacity benefits, denture benefits for the elderly, etc.
Health promotion, for example, funding for cancer screening.
Health insurance can be characterized by two dimensions: the scope of the insurance package indicates how many services and other benefits the Health Insurance Fund finances (list of services). The depth of the insurance package explains to what extent services and benefits are covered by the Health Insurance Fund (how much the Fund pays for the service).
The specifics and extent of non-monetary benefits provided by the Health Insurance Fund are defined in three legal acts, with the most important being the list of healthcare services.
The budget of the Health Insurance Fund consists mainly of the social tax's health insurance portion. It is primarily used to pay for insured individuals' healthcare services and medications. The Health Insurance Fund covers the costs of healthcare services for insured individuals based on agreements with healthcare institutions. The prerequisite for payment is that the service provided by the healthcare institution must be part of the health insurance package (described above).
Contracts are signed with healthcare institutions across Estonia. In allocating the budget for specialized medical care, the number of insured individuals in the region, the number of children under 19 for pediatric dental care, and the number of individuals over 65 for long-term care in the region are considered. Based on this, the Health Insurance Fund enters into agreements with healthcare institutions for the purchase of healthcare services.
The list of healthcare services is a compilation of all medical services, procedures, necessary hospital medications, and other elements included in the health insurance package, along with prices and payment conditions. The list defines which medical services and medications an insured individual can receive and under what conditions and at what cost these services are funded.
The Estonian Health Insurance Fund covers the costs of healthcare services provided to insured individuals based on agreements with healthcare institutions. Payment is contingent upon the service being part of the health insurance package, as described above.
The criteria for changing the list, evaluation conditions, and the process are determined by the Government of the Republic of Estonia. The list of healthcare services is updated annually based on needs and the financial capabilities of health insurance, ensuring that people receive the best possible treatment, considering the evidence-based nature of the treatment (including medical effectiveness) and cost-effectiveness.
The Health Insurance Fund can only pay for those healthcare services that meet specific conditions and are priced according to the regulation of the Government of the Republic of Estonia on the list of healthcare services. As costs for service delivery tools such as equipment, instruments, etc., may change, and healthcare methodologies and organization evolve, funding must keep pace. Therefore, the selection and prices of healthcare services need to be constantly updated. To make decisions about changes, collaboration with specialists in the field, involvement of experts, and comprehensive analyses are conducted. The updating of the list of healthcare services is done in cooperation with general practitioners, hospitals, and specialists.
In order for the Health Insurance Fund to pay for the treatment of insured individuals, it is necessary to establish a price for each healthcare service.
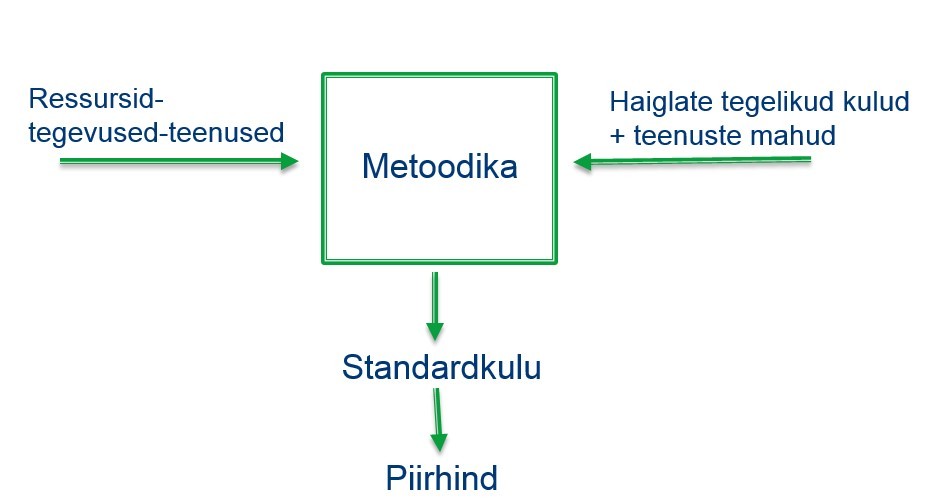
The formation of healthcare service prices must be justified and understandable to various stakeholders. The most significant challenge is to find the optimal price. For this purpose, a unified pricing methodology has been established, based on activity-based costing principles (ABC methodology). This involves describing the activities required for providing a specific healthcare service and, in turn, the resources needed for these activities (e.g., the time of doctors and nurses, equipment). The descriptions of services are based on the actual practices of healthcare institutions.
Services are always described in collaboration with professional associations. These associations provide information on the duration of service provision (e.g., 100 minutes), the number of people providing the service (e.g., two doctors, two nurses, one caregiver), the room where the service is provided (e.g., operating room), the equipment required for service provision (e.g., ultrasound machine), and the disposable tools needed (e.g., syringes). Agreements are also made on the annual usage of these resources (e.g., the ultrasound machine is used for ten years, five days a week, eight hours a day).
Once this information is obtained from professional associations, healthcare institutions are asked for the acquisition costs of all resources. Information is not requested regarding medical staff salaries, as the minimum wage stipulated by the collective agreement is used as a basis. This is multiplied by a coefficient to allow healthcare institutions to pay higher wages than the minimum wage. Data is collected from institutions that provide the relevant services on the largest scale to get an overview of the actual prices in the entire system. After finding the descriptions or standard costs, personnel costs and one-time costs are cross-checked to understand if the descriptions accurately reflect actual personnel and material costs. Healthcare institutions' data on personnel numbers and total costs, along with statistics on provided services, are used for this purpose. Descriptions are adjusted as needed based on the results.
In addition to the components necessary for providing the service, all service prices also include overhead costs (e.g., space costs, utilities, management expenses, IT costs).
The aim of pricing is to ensure that health insurance funds are used efficiently and effectively. The Health Insurance Fund works towards establishing clear and transparent methodologies for determining optimal prices for each healthcare service. We prioritize the continuous development of pricing for medical services as it ensures better outcomes in the delivery of services
